Types of contraception - hormonal, non-hormonal and their forms
Currently, the company has numerous variants in the field of contraceptive methods, which people could only wonder about in the past. The differences between them are reflected not only in side effects and positives, but also in the application procedure of individual types of contraception. However, despite the fact that contraception and pregnancy should be mutually exclusive, this is not necessarily the case. The essential difference between the means to prevent unplanned pregnancy is precisely the effectiveness of the given contraceptive.
Contraceptive options are constantly evolving and emerging, so it is very important to talk about what options we currently have access to, but also how they differ and what potential side effects they have. In our article, in addition to the aforementioned, you will read about the exact division of contraception into hormonal and non-hormonal, while we will also present natural ways of preventing pregnancy. However, we will also answer the very important question of how long contraception works.
What is contraception?
When the word "contraception" is mentioned, most people automatically think of the pill or the classic condom. Contraception used to prevent unplanned pregnancy, however, currently comes in various forms, which are differentiated by their effectiveness in the field of protection, side effects, but also positive effects on the woman's organism or the exact time limit, since when a particular contraceptive works.

Contraception and its types
How contraception works depends largely on its type. Therefore, first of all, we must state the basic division, from which the individual features of the contraceptive method are derived. Contraception is primarily divided on the basis of gender, i.e. male and female. Subsequently, however, individual types of contraception can also be divided into natural, hormonal, chemical or barrier, while this division indicates the aforementioned principle.
What kind of contraception a woman uses is a decision she should review with the help of a gynecologist. It is the professional opinion and insight into the woman's previous medical history that will help in choosing a suitable form of contraception, which will have high efficiency, but minimal negative impact on the health or everyday life of the woman.
The Pearl index, which serves as an evaluation element in the reliability of contraception, can potentially help to choose the best contraceptive method. The value of this index is obtained on the basis of a sample of 100 women using the same method of contraception, in which the number of pregnancies is monitored during one year. The number works on the principle of indirect proportionality, so the lower the given value is, the more effective the method is.
Hormonal contraceptives
As the name implies, hormonal contraception works on the principle of influencing the level of hormones in the female organism in the sense of protection against unwanted pregnancy. A woman's body is a kind of contraception supplied with artificially synthesized hormones that stop the ovulation process, complicate the passage of sperm by thickening the mucus of the cervix, and thus also create a kind of "inhospitable" environment for the fertilization of the egg and its further development in the uterus.
Hormonal contraception comes with many side effects, mainly because all these methods of preventing unwanted pregnancy significantly affect female hormones. This fact is often reflected in the health of a woman's skin and her fluctuating weight, although it can also manifest itself in the form of physiological reactions of the female organism to changes in hormonal levels.
The application of hormonal forms of contraception is diverse, e.g. oral in the form of a pill, injectable, vaginal, but it is also possible to choose among contraceptive methods, such as subcutaneous implants or patches on the skin.

Birth control pills
Oral contraception is considered the most widespread type of prescription contraception. By swallowing the pill, hormones preventing ovulation are released in the body. Because of their influence, a condition similar to pregnancy is created in the female body, which consists in the absence of egg release. Contraception in the form of pills does not stop the maturing of the uterine lining, and thus the female cycle continues, but without significant symptoms, as is usually the case without contraception.
Regularity of use plays a very important role in contraceptive pills. How is such contraception even taken? An essential factor is taking the pills at the same time every day. It is recommended to leave this task for the morning or evening, when the woman will remember the act in question sooner. Gynecologists often recommend taking the first pill on the first day of menstruation, which maintains a certain regularity and the woman has an overview of her cycle and the period of use. However, the use of barrier methods of protection is recommended for at least one month after starting to use contraceptive pills.
After stopping the pills, the full return of menstruation is estimated to take several months after taking the last pill. Pregnancy can also occur during this time, during which the body copes with the sudden restriction of the supply of specific hormones affecting processes in the body.
Contraceptive pills are divided into two subgroups in terms of the hormones contained in the drug. On the one hand, we have combined contraception with the hormones estrogen and progestogen, the main task of which is to stop ovulation, which is helped by estrogen, while on the other hand there is progestogen contraception without estrogen, creating a more complicated passage of sperm into the uterus.
Both types of birth control pills have certain negative side effects that should disappear within about one to three months of starting to take the pills. These include headaches, breast pain, light bleeding or discharge, vomiting, feelings of nausea, but contraception also affects weight gain. It dehydrates the body, which can lead to weight gain. They have a positive effect on acne, premenstrual syndrome, migraine, pain and intensity of menstruation, while also acting as a preventive measure against ovarian or uterine cancer.
We should not forget the extreme cases in which contraception in the form of pills can cause increased blood clotting, which often leads to thrombosis, embolism, heart attack or even stroke. However, based on expert knowledge, cardiovascular diseases are more a consequence of the estrogen component than of the oral form of contraception itself. Therefore, the use of any contraception must be carefully consulted with your doctor.

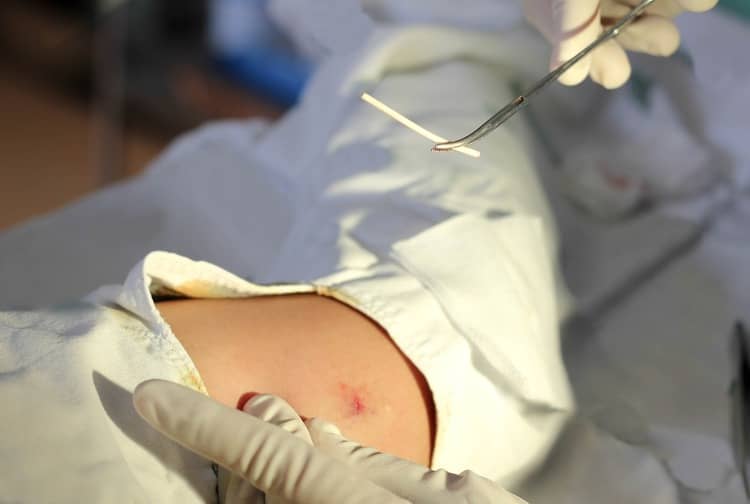
Subcutaneous implant
Doses of the hormone progesterone are released from the subcutaneous contraceptive implant into the bloodstream in the arm, into which this tiny silicone rod is placed under local anesthesia, which thickens the vaginal mucus and thus prevents ovulation. The moment the implant is inserted through a minor procedure, the woman gains protection against conception. The service life and overall functionality of the subcutaneous implant is given in the ratio of three years from a time point of view, while its removal is possible even before the end of this period.
The aspect of effectiveness in connection with this hormonal contraception is stated at the level of 99 percent, while its great advantage is the easing of the menstrual cycle, but also the immediate return of biological processes to their original state after the implant is removed or safety during breastfeeding. Those who are often forgetful will be pleased by the fact that there is no need to remember regular dosing or other contraceptive renewal within this method.
Conversely, irregular menstruation can be considered a negative of the implant, or its complete cessation, the need for medical intervention for its application or side effects in the form of headaches, nausea and rapid mood swings. Contraception also has a negative effect on acne. The contraceptive implant should not be placed in the body of women who suffer from liver problems. A problem liver is not able to process artificial reserves of progesterone, which can lead to the development of benign tumors.
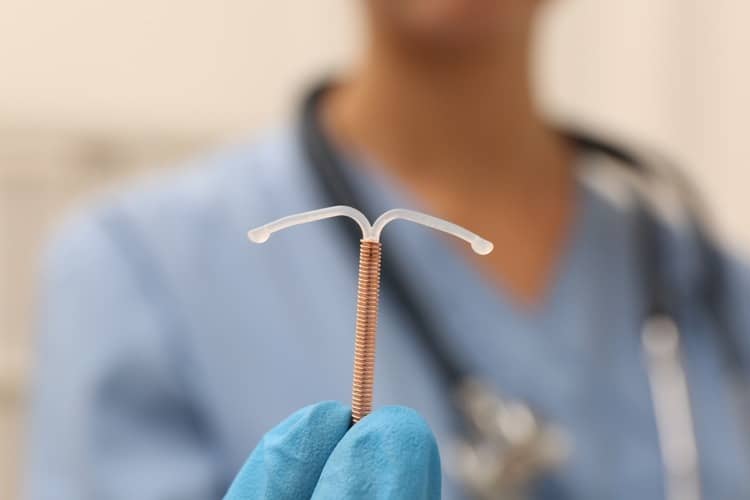
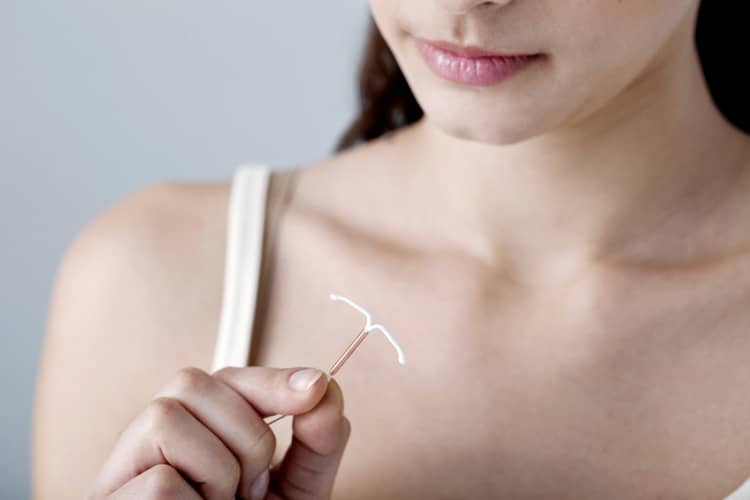
Intrauterine device as contraception
The intrauterine device, and thus the vaginal contraceptive method, is made of plastic, resembles the shape of the letter "T", and is inserted into the woman's body within five minutes with the help of the relevant doctor. In this case, it is a local contraceptive, with the help of which the hormone progesterone affects exclusively the biological processes taking place in a certain area of the female body, namely in the uterus. There, it prevents the preparation of the mucous membrane to create an ideal environment for a fertilized egg, while ovulation takes place without interruption.
The application of the intrauterine device is recommended on the first day after the last menstruation, while the shift or slippage of this contraceptive may occur during the first three months. Almost 100 percent effectiveness is guaranteed by the hormonal body for a maximum of five years, while this form of contraception is recommended for mothers who are no longer planning another pregnancy. However, it is definitely not recommended for women with diseases or other disorders of the uterus.
Both the implant and the intrauterine device have a positive effect on menstrual pain and bleeding during this period of the cycle. A big advantage is the reduction of the probability of uterine cancer, which can be attributed to the body's ability to prevent the rapid reproduction of mucous cells. From the negative point of view, it is necessary to mention mainly breast, head and lower abdominal pain, while mood changes, worsened acne or zero protection against venereal diseases are also characteristic.
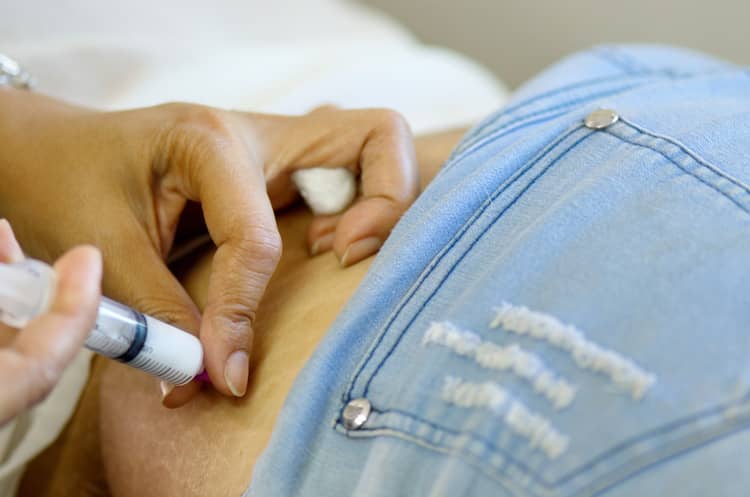
Injectable contraception
Contraception in the form of an injection has the same function as any of the above-mentioned hormonal contraceptive methods. It consists in local application, namely in the shoulder or gluteal muscle. From the injection site, the hormone progesterone contained in the injection dose spreads through the bloodstream, preventing ovulation and sperm penetration. The application is performed by a specialist and one dose works for eight to twelve weeks. If a woman stops using injectable contraception, the return of fertility can take more than 10 months.
The side effects of injectable contraception can be more noticeable than in the case of oral contraception, because unlike pills, which deliver doses of hormones to the woman's body gradually, an injection delivers a larger amount of hormones to the body at once. This can mainly be reflected in changes in taste and subsequent weight gain, mood swings, depressive states, but we also include deviations in libido and nausea among the side effects.
Irregularity of menstruation is completely natural in this case, as it is a relatively invasive form of contraception, which can reduce bleeding and pain during menstruation, but it can also stop it completely, thus throwing the woman's cycle out of balance. However, the probability of uterine cancer is reduced thanks to progesterone.
Vaginal ring
Vaginal contraception literally copying the ring must be inserted into the vagina once a month, while its action and effectiveness can be monitored for the next 21 days. This method belongs to low-hormonal types of contraception and can also be classified as local contraception. Thanks to its softness and flexibility, the ring adapts to the shape of the vagina, while the woman can manage to insert it without help.
Insertion of the vaginal ring copies the female cycle. A woman should insert it into her vagina on the first day of menstruation, and after the period of action has expired, menstrual bleeding will automatically start after its removal. After the end, it is the turn of a new ring and the described process is repeated again. Just like the combined form of the contraceptive pill, the vaginal ring supplies the female body with two types of hormones, namely estrogen and progesterone.
Among the positive aspects, we can mention the improvement of the acne condition, but also the absence of nausea or vomiting due to the method of application, which does not affect the digestive system of the woman in any way. However, the vaginal ring also has a preventive function, especially in connection with the formation of cysts in the ovaries, anemia or uterine cancer. The contraceptive ring is bound to a doctor's prescription, while the replacement dates must be carefully followed.

Contraception in the form of patches
Contraceptive patches work on a similar principle to injectable ones. The patch must be stuck on a clean, non-greasy and intact skin area without hair. The abdomen, shoulder or back area is most often recommended. Such a consistent form of application must be carried out at regular weekly intervals for a period of three weeks. The fourth week is reserved for menstruation, so you do not stick the patch.
Fears about losing the patch are unjustified, because from the material aspect it is a "sticker" capable of overcoming adverse conditions in the form of sweating, showering or swimming. Again, it is a contraceptive containing two types of hormones, which enter the bloodstream through the skin itself, and their main role is to stop ovulation.
Side effects of contraception in the form of nausea and vomiting are excluded thanks to the application that does not involve the digestive tract. The positive effect of the patch can also be noticed on the condition of acne, but also on the alleviation of premenstrual syndrome. It has a preventive effect in the area of anemia, cysts or ovarian cancer. Among the negatives, the need for regular replacement, the possibility of unwanted effects due to hormonal contraception and the price is higher than in the case of contraceptive pills.

Non-hormonal contraception
In contrast to hormonal contraception, it is a type of protection against unwanted pregnancy that should not fundamentally interfere with the female organism. In this group we include natural forms of contraception, but also chemical and mechanical, respectively. barrier contraceptive methods. While barrier and chemical methods of contraception consist in some kind of protective means preventing simple conception, natural methods are based on knowledge of one's own body and the processes taking place in it.
Non-hormonal intrauterine device
The difference between a hormonal and a non-hormonal IUD stems from the structure of the body itself, and thus also the role it performs in the female body. While the plastic hormonal body releases progesterone into the body, the non-hormonal variant has, in addition to the plastic part, a copper wire, thanks to which copper penetrates the uterine lining, creating an inhospitable environment for sperm survival.
Many women choose this contraceptive method because of the five-year protection that the non-hormonal IUD offers, while there is no disruption of intimate life or fluctuations in hormonal levels. This method of contraception is also safe during breastfeeding. On the other hand, however, you need to prepare for stronger menstrual symptoms, which will subside after three to six months.
Since the body contains a significant amount of copper, there is a certain chance that a woman will get an infection after using contraception. A foreign object can move in a woman's body at any time, and it can be completely expelled, so it is important for the doctor to describe to the woman in advance how to check the presence or correct placement of the object. Such a body does not create any barrier, which means that prevention against venereal diseases is zero.
Condom in the role of male contraception
Contraception for men in the form of a latex condom is one of the barrier methods. With the correct use of this contraceptive method, it is possible to prevent an unwanted pregnancy with a probability of almost 90 percent. Since the condom serves as a covering of the male genital organ, there is no clash of body secretions or skin contact. In this case, it is not only about protection in the sense of preventing pregnancy, but also from the point of view of transmission of sexually transmitted diseases.
Condoms are one of the most affordable types of contraception, which can be found in many stores and drugstores. The advantage is also the affordability, while apart from the possible allergy to latex, it does not come with any side effects affecting any of the partners. The disadvantage is the absence of direct skin contact, which reduces sensitivity and in a certain way affects intimacy.
Pesar and female contraception
In addition to male condoms, there are also female condoms, but they are nowhere near as popular as the male version of latex birth control. The application of contraception is somewhat more complicated compared to the male condom, while there are more effective forms of protection. Female condoms are suitable for women whose partners refuse to use a condom, which leads to increased protection against sexually transmitted diseases.
The so-called also works on a similar principle. a pessary, i.e. a flexible silicone cup designed to be inserted into the deeper part of the vagina so as to "barricade" the opening of the cervix for effective protection against sperm penetration into the uterus. It does not contain any hormones and is not noticeable during intimate moments. Pesar excels in its simplicity, and in the case of exemplary care, it can also be reused for a period of two years.
In combination with a spermicidal gel affecting sperm motility, the pessary is an even more effective contraceptive method. A rather acidic gel must be applied to the surface of the silicone bowl before applying it. It should be remembered that it is not a perfect protection against transmissible diseases and sometimes during more passionate love-making it can be released from its original place. If it has not been released and sexual intercourse is over, it is recommended to wait at least six hours before removing the contraceptive from the vagina.

Chemical methods to prevent unplanned pregnancy
We include in this category any special foams, creams, gels or vaginal suppositories that have a major effect on the mobility of sperm, by creating an unfavorable environment for their functioning and survival in the female body. The disadvantage is the absence of protection against communicable diseases, therefore a combination of chemical contraception with effective barrier methods is necessary. Some women may even show some signs of irritation of the vaginal mucosa.
Disposable contraceptive sponge
The contraceptive sponge, like a pessary, is applied a maximum of a few hours before sexual intercourse, while it also mechanically prevents any penetration of sperm into the uterus. However, while the pessary is recommended to be used in combination with a spermicidal gel, the sponge is already pre-soaked with the substances contained in such a gel. Its one-time use consists in immobilizing spermatozoa and preventing them from entering the deeper recesses of the female genital tract. Removing the sponge is recommended at least six hours after sexual intercourse.
The disposable contraceptive sponge for vaginal application is a contraceptive without a medical prescription. It stands out for its simple application and zero sensitivity during sexual intercourse. The introduction can also be carried out the day before sexual intercourse, while in the next 24 hours it is acceptable to have numerous intimate moments without the need to change the sponge. However, the sponge does not protect against sexually transmitted diseases and the substances contained in it can irritate the vaginal mucosa. In some cases, vaginal moisture also soaks into the sponge, which makes it necessary to use a lubricating gel.

Natural contraception
Natural methods of contraception consist in knowing and constantly examining one's own body, or physiological processes taking place in the body. In this category we include a detailed overview of the female cycle, either in the form of counting fertile days or regular basal temperature measurement. Thanks to these forms of contraception, the body is not burdened by hormones, a woman can enjoy direct contact during lovemaking, but during precisely calculated fertile days she still has to resort to other methods of contraception.
Contraception in the form of interrupted intercourse requires consistency, high attention and especially self-control. All these attributes must be fulfilled especially by the partner, who must estimate the right time to pull the penis out of the vagina, in order to avoid ejaculation near the female genitalia. It is not advisable to rely on this form of contraception, because up to a fifth of couples who have intermittent intercourse will become pregnant.
Another natural form of contraception is breastfeeding, during which the body produces the hormone prolactin, which supports the production of breast milk and also prevents the maturation of eggs. Breastfeeding is an unreliable contraceptive method that can only be used during the first six months after giving birth, or until the arrival of the menses. The regularity of breastfeeding is important, consisting in carrying out such feeding of the baby every three hours. However, it should be remembered that this hormone is only released when the baby touches the nipple. This means that no milk pumping or other "tricks" to confuse the organism work.
Contraception after intercourse
The "after" pill is an over-the-counter emergency contraceptive that has a certain time limit for its use due to its effectiveness. After sexual intercourse of an unprotected nature, in which no form of contraception was used or the chosen method of protection failed, it is necessary to take the "after" pill within 72 hours to prevent unwanted fertilization. By the end of the first 24 hours after sexual intercourse, its effectiveness is estimated at 95 percent, while it gradually decreases as the hours pass. This type of contraception is not intended for regular and frequent use, because one dose contains too many hormones that could negatively affect the female cycle and other processes in the female body.
Adverse effects of contraception due to other factors
Combining different medications to treat different problems is generally not recommended. Therefore, the question arises whether antibiotics have any effect on contraception. The answer in this case is negative. Most antibiotics tolerate birth control pills very well, and there are no adverse effects, either in the direction of antibiotic treatment or in the care of protection against pregnancy. The exception is antibiotics for the treatment of tuberculosis, which effectively reduce hormone levels.
Smoking in combination with hormonal contraception can cause certain problems in a woman's life. It is precisely the smokers who belong to the risk group, in which the doctor must really consider whether to prescribe contraceptive pills at all. Therefore, under no circumstances should a woman lie to a doctor about her bad habits. For example, in women over 35 who smoke 15 or more cigarettes a day, there is a sufficiently large contraindication in terms of combined hormonal contraception. Smoking increases the likelihood of cardiovascular diseases, the risk of which is also increased by the hormones contained in contraception.
Alcohol as a bad habit is not an obstacle in connection with the use of contraception, but it can lead to more frequent forgetfulness, which can lead to unwanted pregnancy due to forgotten contraception. If a woman were to take it in time, in a drunken state, it may happen that she will expel it from her body due to nausea along with vomiting, and thus the contraceptive intake will lose its effect.

Menopause and contraception
Using contraception after the age of 40 or 50 does not have to be exclusively associated with preventing unwanted pregnancy. It may be related to coping with the processes that take place in the female body during menopause. The best hormonal contraception for mature women is combined oral contraception with a low estrogen content Birth control pills during menopause contribute to more regular menstruation, but they also help in the fight against unpleasant hot flashes.
Protection in the form of an intrauterine device for older women does help with menstrual bleeding, but it does not eliminate hot flashes. Barrier methods are, of course, recommended for sexual intercourse, while natural methods of contraception, such as counting fertile days, are unreliable due to significant fluctuations in the menstrual cycle. Women in menopause are advised to stop using hormonal contraception, because older age can increase the risk of breast cancer, heart attack or stroke.
Intrauterine device as contraception - experience
On discussion forums, you will encounter many questions regarding the review of a specific form of contraception. Although the answers vary, many times the prevailing opinion is that no form of contraception is 100 percent reliable. A perfect example is the question regarding contraception in the form of the Dana intrauterine device, which was recommended to a woman by her gynecologist for 100 percent effectiveness in case of proper insertion.
A significant majority of the discussing women immediately refuted this claim, because there are women close to them who became pregnant within a few months after the introduction of the body. Such a situation even occurred in the lives of some women even after the age of 40. However, there were also reactions that confirmed the high effectiveness of contraception by stating that they did not conceive, and that they already have a third body. It can therefore be concluded that it is a contraceptive where individuality dominates, mainly because of possible non-acceptance, or rejection of a foreign body by the woman's body itself.
The most frequent questions - FAQ
As can be seen, the topic of contraception and its types is a very extensive issue that needs to be talked about in order to prevent the occurrence of unwanted pregnancies and to spread awareness regarding the side effects characteristic of specific types of contraception. We tried to fit all the most important aspects of the given topic into the main text, while we had to reserve space for additional points of interest in the question and answer section. Our readers can send any other comments or questions to the comments section.
How does Slovak legislation work in relation to prescription contraception?
What all should play a role in choosing a suitable form of contraception?
Is it possible to reverse the sterilization of a man or a woman?
Can the use of hormonal contraception lead to infertility?
Is Norethisterone a contraceptive?
Gallery
Pridať komentár