
Gestational diabetes and the effect on the child. The symptoms will be alleviated by a proper diet
Gestational diabetes or gestational diabetes is one of the relatively common accompanying diseases of pregnancy. Based on statistics, gestational diabetes affects approximately 2 to 5% of pregnancies. Some research indicates the occurrence in up to 15% of pregnant women. This disease causes an increase in blood sugar. The experience of gestational diabetes is different for women. The impact on the child and possible risks for the mother are most often discussed in connection with gestational diabetes. There are also risk factors that increase the risk of developing diabetes in a pregnant woman. How does gestational diabetes manifest itself and what are its symptoms? What should I eat if I have gestational diabetes? Is it necessary to undergo an examination for the diagnosis of gestational diabetes?
- What is gestational diabetes?
- What causes gestational diabetes?
- Symptoms of diabetes in pregnancy
- Gestational diabetes examination and diagnosis – OGTT
- Treatment of gestational diabetes
- Menu or diet during gestational diabetes
- Gestational diabetes - impact on the child and mother
- Gestational diabetes - experience
- The most frequent questions - FAQ
- Comments
Gestational diabetes can have various causes. However, why the problem of lack of insulin, which is supposed to regulate the blood sugar level, appears during pregnancy is not entirely clear. It is most likely the activity of pregnancy hormones in the body. Pregnant women are tested for gestational diabetes between 24-28 weeks. An OGTT - oral glucose tolerance test and blood sampling is performed. If risk factors are present, the test for gestational diabetes can be performed earlier during the 1st trimester. What OGTT values indicate gestational diabetes? Will diet help with gestational diabetes? What are the risks of gestational diabetes for the child?
What is gestational diabetes?
Gestational diabetes or gestational diabetes mellitus is referred to as a metabolic disease that causes the female body to be unable to produce the hormone insulin during pregnancy. It is responsible for regulating blood sugar levels. This type of diabetes is detected exclusively during pregnancy and naturally subsides after childbirth or during the six-month period. Due to changes in a woman's metabolism during pregnancy, sugar is generally absorbed more slowly, and a slightly elevated blood sugar level does not necessarily mean that it is gestational diabetes.
Several factors are behind the development of this disease in pregnant women, while in some cases the predisposition to the development of diabetes is greater. Diagnosis usually takes place around the 24th to 28th week of pregnancy. It is expected to occur around the 24th to 30th week (second half of pregnancy). If some of the risk factors are present in a woman, it is advisable to undergo an examination for gestational diabetes during the 1st trimester. That is why the first examination is sometimes carried out as a preventive measure as early as the 14th week of pregnancy. The examination of gestational diabetes should not be underestimated. Gestational diabetes can affect both the child and the health of the mother.

What causes gestational diabetes?
Why gestational diabetes occurs in pregnant women is a complicated and complex matter. It is primarily a genetic - congenital predisposition. Furthermore, there are profile hormonal changes during pregnancy that can reduce the body's sensitivity to insulin. The role of hormonal changes is to ensure the healthy development of the fetus and maintain the pregnancy.
Some hormonal changes have a negative effect on the production of insulin, which regulates blood sugar levels and contributes to the distribution of glucose into the body's cells. Fluctuations in the blood sugar level and the values are not optimal are typical for improper regulation. Slight deviations in the measurement may not indicate the onset of gestational diabetes, but if the examination shows that the sugar level rises above a certain value, it is gestational diabetes.
Risk factors for the development of gestational diabetes
Certain risk factors can also significantly contribute to the development of gestational diabetes. Based on practical experience, these aspects may be behind the higher probability of developing gestational diabetes. At the same time, the principle applies that if the presence of any of the risk factors in a pregnant woman is obvious, an examination with the help of an oral glucose tolerance test should be performed by the 14th-16th week of pregnancy. Which factors increase the risk of diabetes in pregnancy?
- Age over 30 years,
- overweight or obesity,
- occurrence of diabetes in the family – genetic predisposition,
- gestational diabetes present in a previous pregnancy,
- previous birth of a child weighing more than 4 kg,
- high blood pressure,
- occurrence of repeated miscarriages in previous pregnancies - e.g. biochemical pregnancies,
- unhealthy lifestyle - bad eating habits, sedentary lifestyle, stress,
- occurrence of diseases causing insulin resistance - PCOS (polycystic ovary syndrome).

Symptoms of diabetes in pregnancy
Gestational diabetes usually begins to manifest itself after the 24th week of pregnancy. It is during this period that it is recommended to undergo a laboratory examination. Manifestations of gestational diabetes, or its symptoms are very unremarkable. Increased glycemia, increased blood pressure, more frequent urge to urinate or excessive thirst. The symptoms of such a disease are quite difficult to notice during pregnancy. The symptoms of gestational diabetes can also include more frequent urinary tract infections or inflammatory or fungal diseases of the vagina, which are caused by sugar in the urine that the body cannot process.
The biggest risk of gestational diabetes for pregnant women is that it does not hurt, and many women do not even experience significant symptoms of this metabolic disease. After being diagnosed with gestational diabetes, most women do not even know they have it. They often attribute the symptoms to pregnancy sickness or other processes during pregnancy. It is all the more important to undergo a laboratory examination of gestational diabetes.
Gestational diabetes examination and diagnosis – OGTT
Diagnostics - examination of gestational diabetes is carried out by blood sampling and a glucose tolerance test, in the form of the so-called OGTT – oral glucose tolerance test. In most cases, such an examination is carried out in the 24th-28th week of pregnancy in order to rule out the presence of gestational diabetes in pregnancy at this stage of pregnancy. In some cases, especially if risk factors are present, laboratory blood sampling is carried out before the 14th week of pregnancy to monitor the blood sugar level. The next examination is carried out in the specified period.
It is a laboratory examination performed by a diabetologist or a gynecologist himself. It consists of taking blood on an empty stomach. Before the OGTT examination, a woman must not eat anything for at least 8-10 hours. Intake of pure water or unsweetened tea is possible without restriction. Also, avoid taking medications before the morning examination. Do not take the test if you are sick or after an injury.
The examination itself takes place in three phases. In the first phase, the woman's blood is taken and the presence of sugar in the blood is examined. If the blood sugar level is below or around 5.1 mmol/l, a glucose preparation is administered, which the woman drinks. If the level is higher, it is advisable to repeat the blood sampling the next day. If the increased level occurs during the next sampling on an empty stomach, this is confirmed gestational diabetes.
In the second phase, the woman is given a glucose solution in a volume of 75 ml (diluted in 250 ml of water). It is very sweet, so drinking it is not pleasant, especially during pregnancy, when the digestive tract is relatively sensitive. Sometimes it is possible to add a few drops of lemon. The solution is given in order to find out how the body can cope with the regulation of blood sugar. After the woman drinks the solution, repeated blood sampling is carried out in one hour. If the blood sugar value after this sampling is above 10.0 mmol/l, it is gestational diabetes. The third blood sampling is carried out in another 60 minutes, i.e. 2 hours after the ingestion of the glucose solution, if it shows a value equal to or higher than 7.8 mmol/l, it is also a diagnosed gestational diabetes.
Treatment of gestational diabetes
In more than 90% of cases, it is sufficient to adapt the menu to gestational diabetes. Setting a suitable diet and avoiding certain foods is usually more than enough to alleviate the symptoms of gestational diabetes. Add to this active movement and a certain diet. Definitely do not ignore the treatment. If lifestyle changes do not work and elevated blood sugar levels persist, it will be necessary to proceed with insulin treatment. In pregnant women, it is not possible to regulate the insulin level with pills, so an insulin pen (by injection) is used to deliver insulin to the body. There is short-acting insulin, which a woman injects several times a day, at least 30 minutes before the main meal, or long-acting insulin, which a woman injects once a day. For example, night insulin at 10 o'clock.
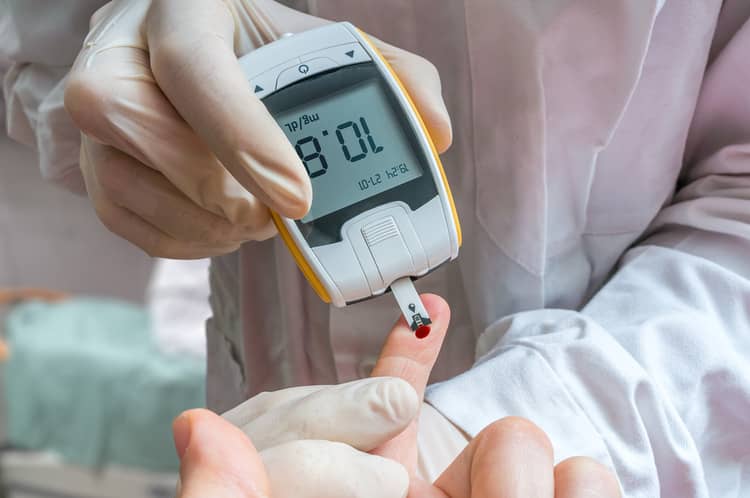
At the same time, there is no need to worry. By following the lifestyle, regimen measures and possible insulin treatment, most women will give birth to a healthy child. Pregnancy with gestational diabetes is always classified as high-risk. So you have to prepare for regular checks and self-check is also important. A glucometer is used to measure blood sugar. You should not forget to check up even after childbirth. It is necessary to undergo an OGTT examination for glucose tolerance approximately half a year after giving birth. Thanks to this, it is possible to confirm whether it was exclusively gestational diabetes or whether the increased blood sugar level persists and it will be necessary to establish a suitable therapy - insulin treatment.
Menu or diet during gestational diabetes
When it comes to eating, it is generally recommended to limit daily intake to 200 g of carbohydrates, 80 g of protein and 30 g of fiber. Of course, not every mom has the need to count calories. In that case, stick to certain principles related to the adjustment of eating habits. Proteins should ideally come from dairy products or lean meat (chicken, turkey). Fats should be primarily of vegetable origin. Follow the correct diet during pregnancy and divide your food into 5 to 7 small portions a day. Try to stick to these following principles as well.
- Limit sweets - sweets, jams, toppings, wafers, cakes, compotes, desserts or chocolates. Give preference to less sweet fruits - white grapes, melon, mango, raspberries, currants.
- Prefer pure dairy products without flavorings. Therefore, prefer white yogurt to apricot yogurt. From dairy products, focus more on low-fat milk cheeses or cottage cheese.
- No fried foods or cured meats. Prefer lean chicken, turkey or rabbit meat or fish (preferably freshwater). Eggs are also a good source of protein. Some nuts (watch out for allergies), seeds or cold-pressed vegetable oils are also suitable for fat intake.
- For fiber intake, it is advisable to include lettuce, zucchini, spinach, asparagus, beetroot, carrots, sweet potatoes (sources of carbohydrates) in your diet. Instead, limit the starch found in potatoes, rice, cereals or pasta. Buckwheat, bulgur, stewed vegetables, whole grain bread or legumes are very good alternative side dishes.
- No sugary drinks or sugary teas. It goes without saying that alcohol is omitted.
- Dia products, which are commonly consumed by diabetics, are not intended for pregnant women. They are intended for people with standard diagnosed diabetes.
If a woman suffers from gestational diabetes, it is necessary to monitor the blood sugar level after a meal and write down the values. You can use a glucometer for this purpose and measure the values accurately on an empty stomach or after a meal. Fasting glycemia should be less than 5.3 mmol. One hour after a meal, the level should not exceed 7.8 mmol/l, and two hours after a meal, it should be less than 6.7 mmol/l. Women who are in the phase where it is necessary to inject insulin should measure their blood sugar level at least 4 times a day.

Daily exercise is very important, even if it is just walking. In addition to walking, swimming or yoga is also very good. Avoid pressure exercises or contact sports where there is a risk of falling or hitting. Never lie down immediately after eating. Resting after a meal can lead to an increase in blood sugar.
Gestational diabetes - impact on the child and mother
The risks associated with gestational diabetes are very specific and individual for each pregnancy. In any case, there are several known risks that primarily untreated gestational diabetes entails. Diagnosis and treatment are crucial precisely in order to avoid the following complications and consequences.
Pregnant women diagnosed with gestational diabetes have a 50 to 60 percent chance of developing type 2 diabetes within 10 to 15 years. There is also a high assumption that if a woman had gestational diabetes in her first pregnancy, it will accompany her during subsequent pregnancies as well. Untreated gestational diabetes increases blood pressure, there is a greater risk of vaginal infections, and complications can also arise during childbirth. A common case is the development of preeclampsia, which is a disease that causes swelling and high blood pressure, which can lead to problems with the supply of nutrients to the fetus.
It is often assumed that pregnant women with diabetes have a high risk of developing developmental defects in the child, but the fact is that this risk is higher if the woman was diagnosed with diabetes before pregnancy. Gestational diabetes does not increase this risk, because it arises only in the second half of pregnancy, when essential development of the fetus has already taken place. However, it can to some extent influence the onset of obesity in a child at a later age.
For the baby, untreated gestational diabetes can mean a more serious course of neonatal jaundice. It is also very common that gestational diabetes causes an accelerated increase in the weight of the fetus, and children with a higher birth weight of more than 4,000 g are often born. This can lead to complications during childbirth, such as a forced caesarean section. Newborns also have a state of hypoglycemia, which is a lack of sugar in the blood. After birth, breathing problems may appear in children due to insufficient development of internal organs, and calcium deficiency is also common. A child born to a mother with untreated diabetes is also called a newborn of a diabetic mother. An untreated condition can be fatal and lead to the death of the fetus in the womb due to the aforementioned immaturity of the internal organs.
Gestational diabetes - experience
Most women who have been diagnosed with this condition refer to the need to maintain a proper lifestyle and adjust their eating habits. Despite this, many mothers are afraid. Other discussants with experience with gestational diabetes point to the fact that their child was born without complications and healthy. They consider it important to limit the intake of sweets and overall self-control is essential. In some women, the condition worsened and it was necessary to proceed with insulin treatment. There is also agreement that if diabetes occurred during one pregnancy, it also appears during the second.
The most frequent questions - FAQ
Do you know what gestational diabetes is? Are you pregnant and want to know what the disease is and what are its symptoms? In our article, you will read how the examination takes place and when it is appropriate to undergo it. Do you have experience with gestational diabetes? What was the course of diabetes in your case? We will be happy if you join the discussion below the article and contribute your own opinion. Your advice, recommendations and knowledge can be very helpful for other pregnant women.
What is gestational diabetes?
What causes gestational diabetes?
What is the OGTT test?
Pridať komentár






